By: Rachel Long, PT, DPT
How Physical Therapy for Plantar Fasciitis Can Help You
What is Plantar Fasciitis?
- Plantar fasciitis is inflammation of the thick band of tissues that runs along the bottom of your foot to your toes.
Symptoms of Plantar Fasciitis
- The primary complaint with plantar fasciitis is typically pinpoint tenderness on the heel and occasionally pain or cramping into the arch of the foot. Most often, this pain is worse in the morning following the position that your foot is placed in (toes down) by the sheets while sleeping causing a shortening of the plantar fascia. The pain is usually worse with weight-bearing activities including walking, standing, or recreational sports, and may be dependent on the type of footwear vs walking barefoot. Plantar fasciitis can be debilitating without treatment as rest does not typically prevent the symptoms from returning with a return to activity and weight bearing.
Cause of Plantar Fasciitis
- Generally, the cause of plantar fasciitis is insidious or unknown. Risk factors include age (40-60 is most common), obesity, foot mechanics like having flat feet, and working in a service industry that results in prolonged standing on hard surfaces such as healthcare workers, teachers, or cashiers.
Treatment of Plantar Fasciitis
- Treatment of plantar fasciitis should be multi-faceted and may include stretching, strengthening, manual therapy, footwear changes including orthotics, and education for the prevention of future episodes of plantar fasciitis. Physical therapy for plantar fasciitis includes a walking assessment to determine your foot type and any compensatory patterns that may have developed due to complaints of foot pain. Oftentimes, physical therapists will work with podiatrists and orthotists to ensure that you receive all the care necessary to relieve the pain in your foot.
Foot Stretches
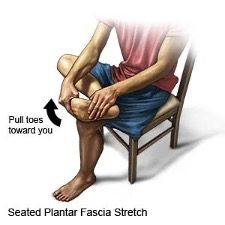
- The most common foot stretch is for the plantar fascia itself and can be completed in a seated position. Sit forward in a chair and place the involved toes on the floor with the heel elevated. Push the heel up toward the ceiling until you feel a gentle stretch across the arch of the foot. Hold 30 seconds. This can also be done with your foot elevated on your opposite knee and using your hand to push the toes back.
Calf Stretches
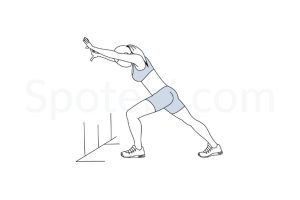
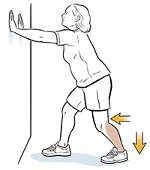
- The calf is a combination of several muscles with the 2 largest being the gastrocnemius and the soleus. To stretch the calf, lunge one foot backward keeping the knee straight and the heel on the ground as you lean forward over your other leg. Hold 30-60 seconds and repeat 3 times. To stretch the soleus, the position is the same with a slight knee bend in the leg you are stretching. Oftentimes, the stretch is felt closer to the heel with the addition of the knee bend.
Foot & Ankle Exercises
- There are many strengthening exercises for the foot and ankle that may be prescribed by your healthcare practitioner depending on the severity of your case, any weakness that may be present, your activity level, available range of motion, and any individual goals you may have. Exercises should be done barefoot if tolerated to allow for increased awareness of the small muscles in your feet that work to protect and reduce stress on the plantar fascia. Generic foot strengthening exercises are listed below.
- Toe Yoga- keeping your foot flat on the floor, lifting only the big toe pull it up off the floor, and keeping the 4 little toes down. Pause 3 seconds. Repeat this movement by pressing the big toe down and lifting the 4 little toes toward the ceiling.
- Foot tenting- keeping your toes and your heel on the ground, lift the arch off the floor. This can be done seated or standing and it may be easier to feel standing. Hold the position for 10 seconds and repeat it 10 times.
- Heel raises- Press all ten toes into the ground and lift your heels up as far as you can slowly. Repeat up to 30 times
- Self-massage- using a tennis ball or frozen water bottle, roll your foot back and forth across the bottom of the foot allowing for gentle massage of the plantar fascia and the muscles on the bottom of your feet.
Orthotics
- You may be prescribed orthotics, or an insole, for your shoe by a podiatrist or suggested orthotics by a physical therapist. Orthotics are placed in the shoe and provide additional support for your foot. These can be over the counter and purchased at a local drugstore, shoe store, or sporting goods store or may be designed by an orthopedist and customized to your foot.
Night Splints
- Night splints can be purchased over the counter at any local drugstore and are helpful in preventing plantar fasciitis pain in the morning. The splints are designed to keep your foot up with the toes toward the ceiling while sleeping allowing the plantar fascia to be stretched throughout the night.
Manual Physical Therapy
- A physical therapist may complete manual therapy or massage along the bottom of your foot and into your Achilles tendon or calf musculature using their hands or various tools to complete Instrument Assisted Soft Tissue massage or Graston techniques. These techniques are often helpful in the management of pain and inflammation in the plantar fascia.
Kinesiology Taping
- Kinesiology tape is a flexible tape that can be placed directly on the skin with a variety of stretch in order to inhibit, facilitate, or support the structure it is placed on. A physical therapist can determine the specific placement and technique for each individual person. Kinesiology tape may be used instead of an orthotic or in addition to an orthotic. One of the benefits is that it is applied directly to the skin and can provide support to the foot when barefoot.
Is Physical Therapy for Plantar Fasciitis Right for You?
- Physical therapy is a conservative treatment method for plantar fasciitis that will utilize a combination of manual therapy, patient education, stretching, and strengthening techniques to reduce your pain. The goals of physical therapy align with the patient to allow you to return to what you love- walking, dancing, golf, tennis, or just getting out of bed without pain. Typically, the earlier you receive treatment, the more quickly the symptoms can be controlled, and compensatory leg or back pain can be prevented. In Pennsylvania, physical therapists are able to see patients without a doctor’s referral, or Direct Access, for up to 30 days.
References
- Matthew Lambert, Rebecca Hitchcock, Kelly Lavallee, Eric Hayford, Russ Morazzini, Amber Wallace, Dakota Conroy & Josh Cleland (2017) The effects of instrument-assisted soft tissue mobilization compared to other interventions on pain and function: a systematic review, Physical Therapy Reviews, 22:1-2, 76-85, DOI: 10.1080/10833196.2017.1304184